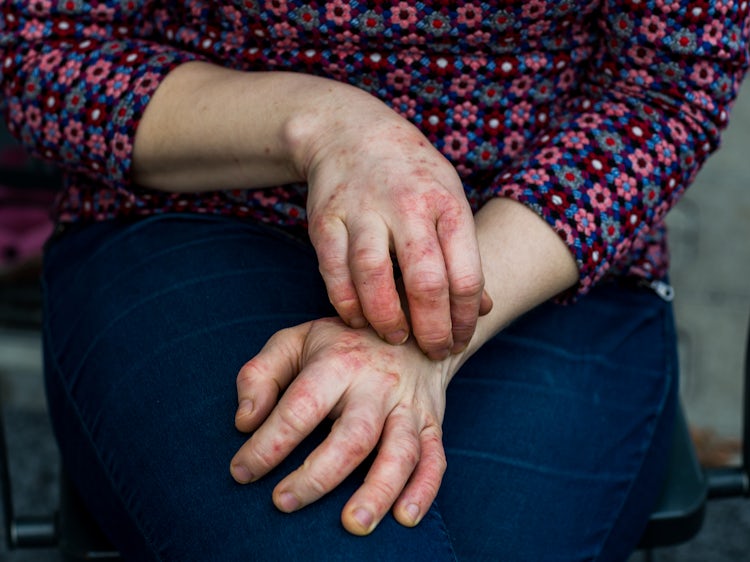
Eksem kan være kronisk (langvarig) eller akutt. De fleste har et forløp med bedring om sommeren og forverring om vinteren. Den kroniske formen av eksem kjennetegnes av et kløende utslett. På grunn av kloring dannes det ofte områder med fortykket hud som lett sprekker. Akutt eksem er preget av rød, hoven og kløende hud, eventuelt med væskefylte blemmer.
Ved eksem er forsvaret mot infeksjon i huden svekket, og ved infeksjoner kan det lett oppstå forverring i eksemet.
Hvilke symptomer gir eksem?
Atopisk eksem: Atopisk eksem er en kronisk tilbakevendende inflammatorisk hudsykdom, som kjennetegnes av kløe og hudsår. Atopi betyr annerledes, i dette tilfellet er det huden som er annerledes. Uttrykket brukes som betegnelse for arvelig betinget allergisk eksem. Sykdommen gir redusert hudbarriere og tørrere hud, og er assosiert med økt nivå av antistoffer kalt IgE i blodet. Atopisk eksem kommer ofte tidlig i livet og de fleste får diagnosen før seks års alder, men den kan også oppstå senere i livet.
Kontakteksem: Kontakteksem som nettopp har oppstått eller blusset opp igjen, fører til rød og hoven hud med små og store blemmer, og væskende sår. Eksemet oppstår på steder som kommer i direkte kontakt med stoffer som huden reagerer på. Hvis kontakteksemet har vart lenge, er huden tørr og sprukket. Sterk kløe er vanlig. I begynnelsen er eksemet begrenset til den delen av huden som har vært i kontakt med det du har reagert på, men etter hvert kan det også spre seg til andre områder på huden.
Seborroisk eksem: Ved seborroisk eksem hos spedbarn er huden fet og rød, med fete skorper i panne, hodebunn, ansikt og hudfolder i nakke og underliv. Hos voksne opptrer dette som rød, fet, flassende hud i sentrale partier i ansiktet, hodebunn, bak ørene og på brystet.
Bleieeksem: Bleieeksem er rødt, med glatt og eventuelt væskende hud i bleieområdet.
Hvem får eksem?
Det antas at cirka 15 prosent av norske barn er rammet av eksem. Sykdommen begynner ofte når barna er noen måneder gamle, og forsvinner hos 60 prosent innen de er fire år. Det kan imidlertid komme igjen senere, i tenårene eller i voksen alder.
Atopisk eksem: Det er først og fremst små barn som får atopisk eksem.
Kontakteksem: Kontakteksem er sjeldent i småbarnsalderen, men fra skolealder er forekomsten økende. Hull i ørene, piercing og bruk av uedelt metall mot huden har ført til en betydelig økning av kontaktallergi mot nikkel
Seborroisk eksem: Seborroisk eksem er relativt vanlig. Eksemet kan oppstå allerede i de første levemåneder, men er vanligst i voksen alder.
Årsaker til eksem
Årsaker til atopisk eksem: Årsaken til atopisk eksem er ukjent. Allergier har betydning for noen, men aldri alene. Dette er en sykdom som er knyttet til arv, genetikk, miljø og livsstil. En ser ofte at også andre familiemedlemmer har såkalte atopiske sykdommer, altså astma, eksem eller allergi.
Rundt 20-30 prosent av personer med atopisk eksem har allergi, og hos noen kan dette ha betydning for eksemet. Forebygging via kosthold hos mor under svangerskapet og etter at barnet er født ser ut til å ha liten påvirkning på utviklingen av atopisk eksem hos barnet. Undersøkelser tyder likevel på at symptomer på atopisk eksem kan utsettes hos noen hvis barnet ammes de første fire til seks levemånedene.
Årsaker til kontakteksem: Kontakteksem oppstår når huden reagerer på stoffer den kommer i kontakt med. Tilstanden kan være både allergisk og ikke-allergisk. Den ikke-allergiske reaksjonen skyldes direkte kontakt med hudirriterende stoffer som rengjøringsmiddel, vann og desinfeksjonsmidler. Den allergiske reaksjonen utløses av allergifremkallende stoffer, som for eksempel nikkel, krom, gummi, formaldehyd eller parfyme.
Årsaker til seborroisk eksem: Seborroisk eksem skyldes ikke overfølsomhet, men er en sykdomsreaksjon i talgkjertlene og kan kanskje skyldes spesielle gjærsopper som normalt finnes på huden. Personer med fet hud og stor talgproduksjon er utsatt for denne eksemtypen.
Årsaker til bleieutslett: Årsaken til bleieutslett er irritasjon fra urin og avføring.
Hvordan få hjelp?
Hvis barnet ditt har lettere tilfeller av forbigående eksem, kan råd og veiledning på helsestasjonen være nok. Hvis det trengs mer behandling, kan du kontakte fastlege som eventuelt henviser videre til spesialist.
Hva kan forverre eksem?
Faktorer som kan forverre eksem er blant annet:
- Stivt og stramt tøy. Barnet vet best selv hvilke tekstiler som klør!
- Grove ullprodukter
- Polyester
- Sterkt farget tøy
- Fuktighet
- Stress
- Infeksjoner
- Næringsmidler
- Klorvann
- Tobakksrøyk
- Parfyme
- Allergier
- Alkaliske såper
- Avfettende kjemikalier
- Varme